KRF Clinical Practice Guidelines in Keloid Disorder (KRF Guidelines®) Facial Keloids Version 1.2018
Michael H. Tirgan, MD
SUMMARY
Diagnosis
Diagnosis of facial keloid lesions is based on clinical history as well as clinical appearance of the skin lesion. A biopsy is almost never indicated to establish the diagnosis.
Grouping of facial keloids
For purposes of this Guideline, facial keloid lesions are divided into four types:
- Early-stage lesions presenting as protruding papules, linear, and nodular lesions (<2 cm-facial stage IA).
- Locally advanced-organized patch presenting as a conglomeration of papules or linear lesions and formation of keloid patches (2-5 cm-facial stage IB).
- Superficially spreading/multifocal disease presenting as large areas of facial involvement (>5 cm in total-facial stage IC and above).
- Tumoral disease presenting as bulky tumor masses.
- Tumoral-(2-5 cm–bulky tumor mass, facial stage IB)
- Tumoral-semi-massive (5-10 cm–bulky tumor mass, facial stage IC)
- Tumoral-massive (>10 cm–bulky tumor mass, facial stage IIA and higher)
Treatment
- Intra-lesional triamcinolone (ILT) is the first-line treatment for all early-stage, papular and linear lesions (see KRF Guideline – ILT).
- Intra-lesional chemotherapy (ILC) should be considered for all early-stage, papular and linear lesions that fail to respond to ILT (See KRF Guideline – ILC).
- Contact-cryotherapy with or without ILT is the preferred and primary method of destruction for all nodular, locally advanced and tumoral facial keloid lesions (See KRF Guideline – Cryotherapy).
Rationale for the use of cryotherapy:
a. Cryotherapy is an effective method of treatment for protruding facial keloids.
b. As opposed to surgery, cryotherapy does not result in worsening of the keloids[1,2].
c. As opposed to surgery, radiation therapy is unnecessary after cryotherapy.
Cryotherapy should be repeated once every 4-8 weeks, depending on the size of the treated lesions. Once all visible keloid
lesions are brought under control, patients should be followed clinically to detect any potential early recurrent disease.
All patients should be instructed to examine their face on a regular basis and return for treatment at the earliest sign of a
potential recurrence or development of new lesions.
Treatm ents to avoid
Surgery shall NOT be used in the treatment of facial keloids. Surgical intervention is a known cause for the worsening of keloids [1, 2] which is also well documented in several cases presented in this guidance.
Surgery may only be considered in cases of massive facial keloids and must only be done in coordination with a specialist physician who is familiar with the treatment of keloid disorder and can implement proper adjuvant medical treatments in an attempt to prevent recurrence.
Radiation therapy shall NOT be used in the treatment of facial keloids. Radiation therapy carries a known risk of causing secondary malignancies [3,4].
Lasers shall NOT be used in treatment of facial keloids. This intervention may result in the worsening of keloids [5].
Overview
This KRF Guideline was developed with the aim to provide:
- General discussion of facial keloids.
- Natural history of facial keloids.
- Classification system for facial keloids.
- Recommendations for treatment and follow up.
Introduction
Keloid involvement of the facial skin is fairly uncommon and occurs in approximately 15 percent of patients with keloid disorder. This pattern of presentation is somewhat gender and race specific.
In a recent analysis of data from 1,088 consecutive patients seen by the author is his keloid specialty practice, there were 157 ( 14.4%) patients with facial involvement. Among these patients: 59 (38%) were female and 98 (62%) were male, 118 (74%) were African-American, and 24 (15%) were Asians.
Clinical presentation of keloid disorder in the face varies by the ethnic background. The tumoral facial keloids are almost exclusively seen among African-Americans. 43 of 45 patients who presented with tumoral keloids were African- American. Table below shows the breakdown of patients according to ethnic background and gender.
The two most common triggering factors for formation of facial keloids are acne among Asians and Caucasians and ingrown facial hair among African-American men. Proper management of these two factors should be incorporated in the plan of care for all patients.
It is with control and/or resolution of acne that most patients will stop developing new keloid lesions. Isotretinoin (Accutane) used to treat acne is a significant contributing factor to development of multifocal keloids in genetically predisposed patients [3].
Involvement of the face as the only site of keloid disorder is uncommon. Of the 157 cases seen by the author, 117 (74.5%) had keloid lesion(s) elsewhere on their skin.
As with other keloids, the clinical presentation, size and shape of facial lesions vary from patient to patient. Facial keloids in their early stages are small and few in number. As time passes, the lesions grow in size and spread to involve larger areas of the face.

Table 1. Baseline characteristics of all patients with facial keloids according to gender and ethnic background.
Overall Treatment Strategy
A few basic principles must be considered as we develop a plan of treatment for keloid patient, especially those with facial keloids:
- Involvement of the face is a dynamic process. Over time, the disease will progress in most patients and will result in the enlargement of the existing lesions.
- The disease process is multifocal. Quite often, patients will form new lesions, either near their original facial keloid(s) or distant from it and in other parts of their skin.
The most important goals of treatment are:
a. To bring the triggering factor under control. Manage acne in all patients and reduce the incidence of ingrown hair in African-American men with curly facial hair by trimming the facial hair as opposed to clean shaving.
b. To intervene very early and to bring the lesions under control with a combination of intra-lesional triamcinolone (ILT)/intra-lesional chemotherapy (ILC) and cryotherapy.
c. To avoid surgery in all patients. Surgical removal of facial keloids – a dynamic and multifocal disease – is an inherently flawed approach that exposes patients to the unnecessary risk of developing massive tumoral keloids.
Treatments to avoid
Surgery shall NOT be used to remove facial keloids. As documented in this Guideline, surgical intervention is a known cause for the worsening of facial keloids [1, 2]. Radiation therapy shall NOT be used in the treatment of facial keloids. This intervention may induce neoplastic transformation of the irradiated tissues [3,4]. Lasers shall NOT be used in used in the treatment of facial keloids. This intervention may result in the worsening of keloids [5].
Early-stage Facial Keloids
Facial keloids at their earliest stages appear in two distinct manners:
Protruding papule(s) that often form on the jawline and are triggered by acne or ingrown facial hair (Figure 1).
Linear keloid lesions that often form near the jawline (Figure 2, 3).

Figure 1. Early-stage involvement of face with keloid disorder presenting with several small protruding papules clustered near the jawline.

Figure 2. Early-stage linear keloid in a young Asian female.

Figure 3. Early-stage linear keloid in a young African-American male.
Treatment
There are two distinct goals for treatment of patients with early-stage facial keloids:
- To induce remission.
- To prevent progression or worsening of the keloid lesions.
It is of utmost importance to manage these patients in a manner that will prevent formation of large and tumoral keloids. The treating physician and the patient both must be cognizant of the facts that the disorder is multifocal with
It is of utmost importance to manage these patients in a manner that will prevent formation of large and tumoral keloids. The treating physician and the patient both must be cognizant of the facts that the disorder is multifocal with a dynamic pathophysiology and while the triggering factors are still active – with the passage of time while the triggering factors are still present and active – most patients are destined to develop new lesions, either in the same vicinity or elsewhere on the face, or distant parts of the skin. It is naïve to think that the keloid process is static, or is limited to only one segment of the face such that it can be surgically treated.
All keloid patients have to be treated in accordance with a long-term treatment and follow-up plan. Patients also need to be adequately educated about their illness and its biology.
ILT injection is the first-line treatment for all earlystage papular/linear facial keloid lesions (please see KRF Guideline-ILT). The lesions must be followed carefully, and ILT shall be continued on a regular basis to achieve maximum response. Most lesions respond to ILT treatment. It is of equal importance to identify the triggering factors, and in the case of acne, to optimize anti-acne treatment.
Progression of the Early-sta ge Facial Keloids
Over time, the majority of untreated keloid papules or linear lesions will grow to form nodules, or become thicker linear keloids (Figures 4, 5, 6).
For lesions that are on the path to becoming bulky, the author recommends a combination of ILT injections and contact cryotherapy. This combination is an effective treatment that can reduce the mass of keloid(s) over a short period of time. Once the mass of the lesion is reduced, treatment with single-agent ILT should be continued to control the base of the lesion and to prevent recurrence. The frequency of the ILT injections will vary from patient to patient but should be optimized to keep the disease process under control. ILC should be considered for all patients who fail to respond to single-agent ILT or ILT combined with cryotherapy.

Figure 4. Multiple raised keloid papules/early nodules among young African-American females. Notice multifocality of the disease process.

Figure 5. Early-stage, yet bulky linear facial keloids in a young Asian female.

Figure 6. A 25-year-old Asian female with progressive early-stage facial keloids. Notice presence of the papular and nodular lesions
Locally Advanced Facial Keloids
If left untreated, or if treated incorrectly, the keloid process will progress. This is evidenced by an increase in the number of facial lesions as well as continued growth and the merger of the existing lesions. Progressive facial disease is often coupled with progression of the disease elsewhere on the skin.
Case Study 1
A 41-year-old Caucasian male presented with locally advanced jawline keloid (Figure 7,8) that had started 11 years earlier. He had previously been treated with multiple ILT injections as well as laser treatments. Over the preceding years, he experienced recurrent local infections which was thought to be linked to ingrown facial hair within the keloid mass.
He was started on a course of ILT to all raised and inflamed lesions along with cryotherapy to the raised bulky parts of this lesion.
Treatment was delivered once every 2-3 months to achieve maximum response and then once every 6-9 months to treat recurrent or new lesions.
Figures 9 -11 depict the response that was achieved following treatment with a combination of ILT and cryotherapy. This intervention resulted in a change in the biology and behavior of the disease that for 11 years had caused a constant inflammatory reaction and frequent local infections.

Figure 7. Locally advanced facial keloid in a 41-year-old Caucasian male.

Figure 8. The same patient, small papular facial keloids on the right side of the face at presentation.

Figure 9. The same patient, three years after the initial presentation. Note significant reduction of the inflammatory reaction that was present at initial presentation (Figure 5).
This case exemplifies excellent results that can be achieved with ILT combined with cryotherapy. The small keloid on the right of the face required only one treatment, and has remained in remission for 5 years (Figures 8, 11).
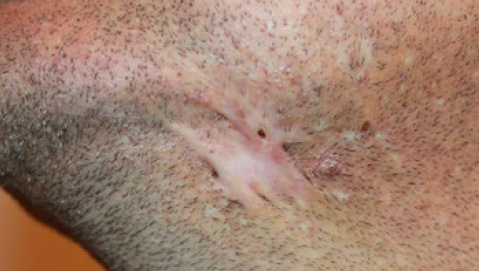
Figure 10. The same patient, 5 years after initiation of ILT and contact cryotherapy. The inflammatory process has now totally subsided, and the keloid process has become dormant.

Figure 11. The same patient, 5 years after initiation of ILT and contact cryotherapy. Total keloid ablation with durable results. Notice two minor marks at the site of the treated keloids.
Case Study 2
A 28-year-old Caucasian female presented with a two centimeter keloid on her chin (Figure 12). She had a scar on her chin that had been excised about a year earlier. That procedure triggered formation of a keloid, which had been removed twice surgically, yet it regrew after each surgery. Her last keloid removal surgery was two months prior to her current presentation. This patient did not have any other keloid lesions.
This lesion was first treated with cryotherapy (Figure 13-15) and subsequently with repeated cycles of ILT and ILC. Remission was achieved 16 months later (Figure 16). Three and a half years later, this lesion still remains in remission.

Figure 12. Nodular facial keloid in a 28-year-old Caucasian female.

Figure 13. The same patient, immediately after application of cryotherapy. The frozen keloid appears white.

Figure 14. The same patient, three weeks after the initial cryotherapy. Notice the significant reduction in the mass of the treated keloid.

Figure 15. The same patient, seven months after the initial presentation.

Figure 16. The same patient, sixteen months after initial presentation. Remission is achieved after several courses of ILT, cryotherapy and ILC.

Figure 17. The same patient 3.5 years after induction of remission with no further post-remission treatments.
Case Study 3
A 28-year-old male presented in February 2013 with a four year history of bilateral facial keloids (Figures 18-19). Prior to his presentation, he had received several ILT injections and had also undergone surgery to remove the keloids from both sides of his face. Unfortunately, the keloids relapsed on both sides, and grew to involve a much wider area of his face.
This patient was treated with a combination of ILT and cryotherapy. Within a few weeks from his first treatment, significant improvement was achieved on both sides of his face (Figure 20). The treatment cycles were continued every 6-8 weeks until much of the disease came under control, and thereafter once every few months. Figure 21 depicts the outcome of treatment 18 months after the initial presentation.
In March 2018 after a 14 month gap in treatment, the patient presented with several areas of regrowth and new keloid formation on his face (Figure 22), mostly outside the previously treated areas. Once again, the recurrence was treated, and responded to repeated cycles of ILT and cryotherapy (Figure 23).

Figure 18. Right jawline keloids in a 28-year-old African-American male (February 2013). Note multifocality of the disease.

Figure 19. Left jawline keloids in the same patient (February 2013). The recurrent keloid shown here was frequently infected and complicated with purulent drainage. Note multifocality of the disease in the periphery of the main keloid mass.

Figure 20. Treatment results shown three weeks after the first cycle of ILT and cryotherapy. Depending on the size of the treated lesions, the scabs remain in place for 2-6 weeks after cryotherapy before they slough off.

Figure 21. 18 months after initial presentation (July 2014). Treatment with ILT and cryotherapy was repeated every few months to manage early recurrence and other new lesions that formed in that time frame.

Figure 22. The same patient after a 14 month gap in treatment (March 2018). Note most disease progression is outside of the previously treated areas.

Figure 23. The same patient, six months after re-treatment with ILC and cryotherapy (September 2018). The disease is once again under control.
As demonstrated in this case, there are two separate phases to the treatment:
- Remission inductions
- Maintenance treatment
Induction treatment with ILT and cryotherapy often needs to be repeated every 4-8 weeks until the disease is brought into remission. The frequency of treatment depends on the response to the treatment, healing time as well as durability of the response. Almost all compliant patients who are at this clinical stage of their illness will respond to induction treatment with ILT and cryotherapy. ILC should be considered for all lesions that fail to respond to ILT and cryotherapy. Once the disease has been brought under control, patients have to monitor their facial skin for recurrent disease, or development of new lesions. The rate and pace of regrowth will determine the frequency of future maintenance treatments, which naturally varies from patient to patient.
Tumoral Facial Keloids
An untreated or poorly treated facial keloid nodule can eventually grow in size and expand three dimensionally to form a tumor. For purposes of this Guideline, tumoral facial keloid lesions are divided into three types:
a. Tumoral – IB (2-5 cm – bulky tumor mass, facial stage IB)
b. Tumoral – semi-massive (5-10 cm – bulky tumor mass, facial stage IC)
c. Tumoral – massive (>10 cm – bulky tumor mass, facial stage IIA and above)
Tumoral facial keloids are almost exclusively seen among African-Americans (Figure 24). Among 45 patients with tumoral facial keloids, only two (4.5%) were non-African- Americans (Table 1). Most patients with tumoral keloids have a history of keloid removal surgery. The injury from surgery to either remove a small facial keloid, or another pathology is what triggers the formation of tumoral keloids. Therapeutic interventions shall aim at preventing tumoral keloids by avoiding surgery in management of early-stage facial keloids.
Table 2. History of prior surgery in patients with tumoral facial keloids.


Figure 24. Several cases of tumoral and semi-massive facial keloids among African-American patients.
Massive Facial Keloids
Massive facial keloids (>10 centimeters in diameter, Facial Stage IIA and above) are almost exclusively seen in African- Americans (13/13) and mostly those who have undergone surgery to remove a prior smaller keloid (10/13). Most of these patients have other keloid lesions elsewhere on their skin (13/13). Figure 25 depicts several cases of massive facial keloids.
Treating these patients is quite challenging as most have already been treated with all available therapeutic interventions. Ideally, one would need to have some form of systemic treatment or a drug that can be administered systemically in order to bring the disease process under control, not only in the facial area but also elsewhere in the skin. Unfortunately, there are no systemic treatments available with none on the horizon.

Figure 25. Few cases of massive tumoral facial keloids in African-Americans.
Case Study 4
A 34-year-old African-American male presented to the author in November 2014, seeking treatment for recurrent keloids on his face and neck (Figure 26).
This patient’s struggles with keloid disorder started with developing a keloid on his anterior chest wall soon after he acquired chicken pox at the age 11. Later on, at the age12/13, he noticed “razor bumps”, i.e. papular keloids, forming on his jawline. He recalled that over subsequent years his jawline lesions grew in number and in size, involving his face and the submental area. These lesions were injected with steroids several times but over time they all grew in size and started to merge.
At the age 21, he underwent a series of laser debulking surgeries. It is of interest to know that he was informed that the laser debulking procedure would reduce the size of his keloids without imposing a risk of recurrence or worsening.
Of course, this proved not to be true. Soon after this procedure, there was recurrence at each laser-treated site.
For a period of about 2 years (from about 2005 to 2007), he stopped all standard treatments and instead, tried various home remedies such as keloid pastes, various creams, snake oil, and compression garments in an attempt to flatten his keloid, but unfortunately the keloid continued to grow.
From 2005 onwards, the keloid tissue developed frequent infections. This was complicated with formation of abscesses within and under the keloid, necessitating frequent and often prolonged courses of oral antibiotics. At one point, due to the severity of the infection, he was admitted to the hospital for treatment with intravenous antibiotics.
In late 2008/early 2009, at the age 29, he underwent a series of three surgeries to remove the massive keloid that had formed on his face and neck (Figure 27). Each surgery was followed by adjuvant radiation therapy. Post operatively, he had also received several injections of high dose ILT.

Figure 26. Recurrent keloids along the surgical excision lines.

Figure 27. Massive neck/facial keloid in the same patient prior to undergoing series of surgery and radiation therapy.
Unfortunately, despite the use of adjuvant radiation therapy and several steroid injections, there was a gradual relapse. This relapse, however, has been slow and the appearance of this young man’s face/neck has remained better compared to prior to his surgery (Figure 28).

Figure 28. Recurrent neck/facial keloid in the same patient within one year from surgery.
This case exemplifies the challenges of treating young patients with facial keloids. Although surgery, and in this case laser surgery, may at first seem to be a reasonable option for removing keloid nodules or a small keloid tumors. But unfortunately, as is shown here, surgery often worsens the condition. Furthermore, adjuvant radiation therapy is also not an absolute solution to the prevention of the recurrence.
As opposed to adjuvant radiation therapy, a more intense and regular follow up plan with early implementation of ILC might result in a better outcome after surgical removal of massive keloids.
Limited Role of surgery
Surgery, using a scalpel or a laser devise, should never beused to remove early-stage, nodular, multi-nodular or evensemi-massive facial tumoral keloids. Surgery is a known triggering factor for formation of much larger facial keloids.
Surgery may only be considered in cases of massive facial keloids, and be only performed in coordination with a specialist physician who is familiar with the keloid disorder and can administer proper adjuvant medical treatments, including ILC, in an attempt to prevent post-operative recurrence. When contemplating surgery for patients with massive keloids, one must be reminded that the lesion that is to be removed was most likely triggered by prior surgical removal of a smaller lesion.
Role Of Cry otherapy
Cryotherapy has limited utility in managing patients with massive facial keloids. Case Study 5 depicts the results that can be expected in these very difficult situations.
Case Study 5
A 31-year-old African-American female with very advanced and widespread keloid disorder presented in April 2014 for consultation and management of her facial and other keloids. By this time, she had already been treated with all available treatment options including surgery, ILT and radiation therapy to her face, chest, pubic area, and other parts of her skin.
Her facial keloids were treated with contact cryotherapy. Long-term result of this intervention is depicted in Figure 29.
Recurrence after Surgery
Recurrence after surgery is real, and affects almost all keloid patients undergoing excisional keloid removal. In a dynamic disease that is multifocal, considering surgery is counterintuitive and quite often harmful to patients. Several cases are presented here in Figures 30-32

Figure 29. A 31-year-old African-American female with very advanced and widespread keloid disorder and massive involvement of her face at presentation (left). Bulky portions of her facial keloid were treated with contact cryotherapy. Durable debulking was achieved following cryotherapy.

Figure 30. Post-operative recurrence along the excision line in an African-American female. Note that this patient has had a prior earlobe keloid removal which has resulted in disfigurement of her earlobe.

Figure 31. A 45-year-old African-American male with recurrent bilateral facial keloids after prior attempts at surgical removal of much smaller keloids and skin grafting.

Figure 32. A 20-year-old African-American female presented with early recurrence at the site of prior surgery. A year earlier at age 19, this young woman was treated with surgery followed by radiation therapy to remove a portion of her facial keloid. Recurrence at the excision site was noticed within 9 months of surgery. This case depicts the totally inappropriate approach to treatment of this young woman. Performing surgery to partially debulk a multifocal disease and exposing a 19-year-old patient to radiation therapy does not achieve much, except for putting the patient at a risk forming a massive keloid at the site of surgery. Exposing young patients to radiation therapy puts them at risk of developing cancer in the future [3-4].
References
- Tirgan, MH. Neck keloids: evaluation of risk factors and recommendation for keloid staging system, F1000 Research, June 28, 2016
- Tirgan, MH. Massive ear keloids: Natural history, evaluation of risk factors and recommendation for preventive measures – A retrospective case series, F1000 Research, October 13, 2016
- Miyahara H, Sato T, Yoshino K. Radiation-induced cancers of the head and neck region. Acta Otolaryngol Suppl. 1998;533:60-4
- Ron E. Cancer risks from medical radiation. Health Phys. 2003 Jul;85(1):47-59.
- Tirgan, MH. Laser Treatment of Keloid Lesions, Efficacy and Side Effects, Results of an on-line survey .Abstract – 2nd International Keloid Symposium, Rome, Italy June 7-8 2018. Full manuscript in press.
