KRF Clinical Practice Guidelines in Keloid Disorder (KRF Guidelines®) Intra-Lesional Triamcinolone, Version 1.2018
Michael H. Tirgan, MD
Background
Intra-lesional triamcinolone (ILT) is the most commonly administered treatment to all keloid patients [1]. Despite its very common use, there are numerous uncertainties about ILT. This Guideline provides for some important practical facts about ILT.
In the United States, triamcinolone is marketed as Kenalog. The product is available in 10mg/ml with the trade name Kenalog-10 and 40 mg/ml with the trade name Kenalog-40.
There is a belief among practitioners who treat keloid patients – that at all times – the highest possible doses of triamcinolone, i.e. Kenalog-40, should be used for intralesional injections. The author has personally reviewed medical records of several patients whose keloids have been injected with Kenalog-40. The author has also interviewed several practitioners who only use Kenalog-40 straight out of the vial in injecting keloids.
It is important to note that the package insert of Kenalog-40 [2] comes with the warning “NOT FOR INTRADERMAL USE.” Furthermore, the package insert states the following:
Kenalog-40 Injection has an extended duration of effect which may be sustained over a period of several weeks. Studies indicate that following a single intramuscular dose of 60 mg to 100 mg of triamcinolone acetonide, adrenal suppression occurs within 24 to 48 hours and then gradually returns to normal, usually in 30 to 40 days. These findings correlate closely with the extended duration of therapeutic action achieved with the drug.
The practice of using Kenalog-40 in treating keloid lesions is not only against the guidance from the manufacturer of the product, it explicitly exposes patients to both localized as well as systemic side effects of this product. It is the author’s opinion that this practice should not be used for intra-lesional injection of keloid lesions.
The author is unaware of any studies to determine proper dosage of ILT or the existence of a dose response correlation.
Indications
ILT is indicated as the first-line treatment of all small papular, mid-sized flat, and linear keloids. ILT should not be used in treating very large or bulky keloid lesions (see KRF Guideline – Treatment Strategy).
Recommended Dosage
As a practical principal that applies to all medications, it is most logical to always use the lowest effective dose of any medication. ILT is no exception to this principal. Therefore, in injecting keloids, the lowest effective dose of triamcinolone should be used. As this dose has never been properly established, the author’s practice is to dilute
Kenalog-10 with normal saline, in a ratio of 1 to 5, i.e. a 20% final product dilution. The final solution will contain 2 milligrams of triamcinolone in one milliliter of the solution that is to be used to inject the keloids.
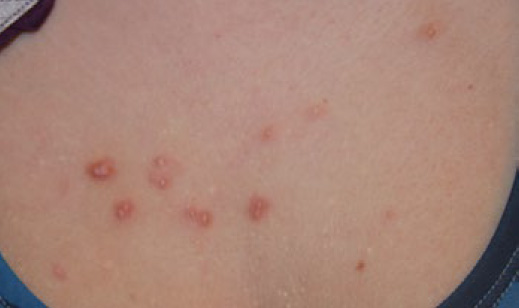
Figure 1. Multiple papular keloid lesions of the chest in a young female before and after treatment with low-dose ILT.

Needle Gauge
The author recommends the Gauge 30 needles for injection of ILT. Larger gauge needles simply introduce a new injury to the keloid that may result in reactivation and worsening of the keloid lesion being treated [4]. Figure 1 depicts the type of needle and syringe that is recommended.

Figure 2. 1 milliliter syringe with gauge 30 needle incorporated in the body of the syringe. This is the most proper type of syringe for ILT injections
Injection Pain
ILT injections can be somewhat painful, especially when given to numerous keloid lesions in one session. Therefore, injection pain needs to be brought up and discussed with all prospective patients. Informing patients about the injection pain reduces the anxiety associated with the first-time injections.
Diluting triamcinolone with normal saline as opposed to lidocaine makes the injections more tolerable. The mild acidic pH of lidocaine results in more discomfort during the ILT injection. Several of the author’s patients who have received both types of dilutions always remind the author not to use lidocaine in preparing their ILT.
Slow and gentle injections as opposed to rushed and quick injections can also make a difference in reducing the discomfort.
For patients who have had prior ILT injections, discussion of the pain from the past injections will guide the treating physician in using methods that will reduce the pain and anxiety from subsequent injections.
Most patients do well with ILT injections. However, there are rare instances of long lasting post-injection pain at the site of injection. For these rare instances, the author dilutes triamcinolone with liposomal bupivacaine which induces durable local anesthesia for up to three days.
Technique and Volume of Injection
Keloid lesions have to be inspected carefully during the injection of ILT. The goal of injection is to deliver a minimal yet sufficient amount of the prepared solution of triamcinolone.
Using the syringe shown in Figure 2, the needle is gently inserted into the body of the keloid lesion. The content of the syringe is gently injected into the keloid to the point of inducing minimal swelling and blanching of the lesion. At this point, the needle is withdrawn. The volume of each injection and number of injections into a given lesion simply depend on the size and thickness of the lesion.
Total dose of ILT needed for lesions that measure up to one centimeter in diameter can usually be delivered in one injection. For long linear or large flat lesions, one has to repeat the injections several times until the whole lesion, or most of it, is injected with an adequate amount of the solution.
A bandage shall be placed over the injected keloid for about an hour.
Assessment of Efficacy
All keloid lesions must be photographed prior to the initiation of any form of treatment, including treatment with ILT, and also during each follow up visit. A pretreatment photograph will serve as a good reference point to determine the efficacy of the treatment.
Upon initiation of ILT, the injected lesion(s) must be inspected within 3-4 weeks, at which point the patient and the provider will together determine whether ILT was effective.
If ILT is felt to have been effective, it can be repeated during this session. Injections should be repeated every 3-4 weeks until maximum response is achieved, at which point the treatment shall be halted and the lesions shall be photographed and observed.
ILT is hardly a curative treatment. In patients who respond to ILT, a determination has to be made as to the ideal frequency of injections to maintain the response. This is done to minimize the total dose of triamcinolone that is delivered to the patient over a given period of time. Patients always are good judges of the duration of efficacy of ILT and shall be consulted to determine the ideal frequency of their injections.
When used in patients with numerous lesions, some lesions will respond better than others. When a lesion achieves a good response, it should no longer be injected.
If ILT is felt to be ineffective after the first injection, it is reasonable to repeat the injection, with the same dose and concentration of triamcinolone, at least one more time. If after two consecutive injections, the patient and the physician determine that ILT was not effective, the treatment with ILT has to be abandoned. There is no justification to use higher doses of ILT, or continue with a treatment that does not show efficacy after 1 or 2 injections. This practice simply exposes patients to undue side effects without added benefit.
ILT is also known to cause worsening of keloids in about 17% of patients [4]. This important fact has to be discussed with all patients prior to initiation of ILT. Patients often have a good sense about the biology of their disease and the pace of growth of their keloid lesions. Any hint of possible worsening of the injected lesions is ground for termination of ILT injections.
Frequency of Injections
When effective, ILT injections often need to be repeated. Most patients who observe improvement in their keloid lesions, also report that the efficacy of the ILT to be temporary and that the lesions, or the symptoms, return after some time [4]. A very small percentage of patients, perhaps those with only one or very few small lesions, may draw long-term benefit and experience durable regression and will not require repeated injections of ILT.
In patients who do respond to treatment and need repeated injections to maintain their benefit from ILT, a determination has to be made as to the longevity of the efficacy, which varies from patient to patient. Future injections have to be given at intervals that match the longevity of the benefit from ILT. The author has encountered patients who only need ILT injection once every six months.
Side Effects
Low-dose ILT, when given as described above, is well tolerated and is free of significant side effects. When used in high doses, i.e. when undiluted Kenalog-40 is injected into the keloids, ILT can cause localized skin atrophy and fat necrosis. It can also lead to systemic side effects such as hyperglycemia, weight gain, cataracts [2], and even Cushing’s Syndrome [5].
Patient depicted below (Figure 3) reported that her dermatologist would take a vial of Kenalog and extract its content into a syringe and directly inject the undiluted medication in her shoulder keloid. Despite lack of efficacy, this practice was continued several times. The patient started noticing weigh gain, at which point she, and not her treating physician, abandoned the treatment with ILT.

Figure 3. 45-year-old female with extensive keloid involving left shoulder. She received six rounds of ILT treatments, once every six weeks, with undiluted Kenalog. She elected to stop treatment (not the physician) once she noticed weight gain, which she (not the physician) attributed to ILT injections. Despite several high dose ILTs, this patient saw absolutely no benefit from this intervention.
References
- Hochman B, Locali RF, Matsuoka PK, Ferreira LM. Intra-lesional triamcinolone acetonide for keloid treatment: a systematic review. Aesth Plast Surg. 2008;32:705-709.
- Package Insert Kenalog-40
- Package Insert, Kenalog-10
- Tirgan, MH. Intra-lesional Steroid Injections: Can they be harmful to some patients? Results of an online survey. International Journal of Keloid Research. 2017 vol. 1 no. 1, July 1, 21-28.
- Sukhumthammarat W, Putthapiban P, Sriphrapradang C. Local Injection of Triamcinolone Acetonide: A Forgotten Aetiology of Cushing’s Syndrome. J Clin Diagn Res. 2017 Jun;11(6).
