Post Otoplasty Keloids - Case Series and Report of Successful Treatment with Cryotherapy
Michael H. Tirgan, MD
ABSTRACT
Background: Otoplasty is a corrective procedure used to reshape the ears, commonly performed on young individuals and even children to improve the appearance, shape, or angle of the ears. Post-otoplasty keloids are known complication of this procedure. Safe and effective treatments are needed for otoplasty induced posterior auricular keloids.
Objective: To review the clinical presentation and natural history of otoplasty induced keloids, and to propose non-surgical intervention with cryotherapy as primary treatment.
Material and methods: This is a retrospective study of 13 consecutive patients with post- otoplasty, posterior auricular keloids who were seen by the author in his keloid specialty practice. Medical records and photographs of the lesions were analyzed. Descriptive statistics are provided.
Intervention:Cryotherapy was the primary treatment for bulky keloids.
Results: Two patients had minimal keloid formation at the sites of otoplasty and were advised to primarily receive, or continue with, intra-lesional steroids. Eleven patients had bulky keloids and were offered cryotherapy as primary treatment. Nine patients consented to the treatment. Three patients are still receiving treatment and as of their last follow-up visit had achieved partial reduction in the mass of their keloids. Six patients completed their course of treatment and achieved desired results with complete or near-complete resolution of their keloids. One patient had minor recurrence and is now undergoing treatment.
Conclusions and Relevance:Using cryotherapy as primary intervention for bulky post-otoplasty keloids can successfully reduce the bulk of these lesions. Cryotherapy seems to not trigger the wound healing response to the extent that surgical scalpels do, therefore resulting in a much better therapeutic outcome. Additionally, cryotherapy is a much less morbid alternative to surgery. It is also less costly and very easy to administer in an out patient setting.
INTRODUCTION
The prominent ear can produce significant social and psychological effects on an individual. Different otoplasty procedures have been described to correct this deformity, quite frequently by way of excision of the posterior ear skin as well as part of the ear cartilage.
A 1994 review by Calder reported 12 cases of keloids and hypertrophic scarring among 562 consecutive cases of otoplasty - an incidence of 2.1%. Nazarian, in his 2011 review of otoplasty, also reported keloids as a longterm complication of this surgical procedure.
Keloids are benign skin tumors that form as a result of a genetically driven dysregulation in wound healing mechanisms. In addition to the genetic predisposition, there must also be an injury to the skin that would trigger the genetically driven, abnormal wound healing response.
Although, for several decades post-otoplasty keloids have been known to occur, there is a paucity of literature as to proper treatment of this unique post-operative complication. Since the triggering factor in development of post-otoplasty keloids is the antecedent corrective surgery, it is counterintuitive to consider surgery as a method of treating these keloids. This paper reports the author’s experience in treating bulky post-otoplasty keloids with cryotherapy as the primary method of treatment.

INSTITUTION
Keloid Research Foundation
CORRESPONDENCE
Michael H. Tirgan, MD
23 West 73rd Street, Suite
GD, New York, NY 10023
htirgan@gmail.com
CONFLICT OF INTEREST
None
FUNDING
None
IRB ASSESSMENT
Determined by central
IRB to be exempt and not
requiring IRB approval.
KEYWORDS
Keloid, cryotherapy,
cryosurgery, otoplasty,
otoplasty complications
MATERIAL AND METHODS
From 2012-2016, thirteen patients with post-otoplasty keloids presented to the author’s keloid specialty medical practice. Baseline characteristics of the patients are summarized in Table 1. Nine patients were male and four were female. The age of the patients ranged from 10 to 39. All patients were Caucasian white or Asian, and none was African American. Only one patient had been previously diagnosed with keloid disorder, and the rest had no keloidal lesions elsewhere on their skin. All patients had undergone bilateral otoplasty anywhere between 1 and 14 years earlier, with the majority (eight patients) having had their otoplasty within the preceding three years. Nine patients had bilateral keloids, and four patients had developed unilateral keloids. Eight patients had previously undergone surgery for removal of their post-otoplasty keloids. The rest of the patients had chosen or had been advised not to undergo surgery. Figure 1 depicts the extent and the appearance of the bilateral keloid lesions in four patients.
Most patients had received a variety of treatments over an extended period of time. The case history of patient RC is quite demonstrative of challenges that these young individuals face for several years after their otoplasty. RC was a 21-year old Caucasian male who was self-referred to the author’s practice in February 2015 with bilateral posterior auricular keloids, depicted in Figure 1, subject # 4. His history dated back to when he was seven years old, at which point he underwent bilateral otoplasty. Within a year, keloids started forming behind both his ears. At the age of eight, he underwent bilateral keloid removal surgery, but within 2-3 months, new onset pruritus signaled recurrence of the keloids. Raised and hard keloids were palpable shortly thereafter on the posterior aspect of both ears. For the next several months, he was treated with monthly intra-lesional steroid injections. However, despite this rigorous treatment, keloids continued to grow. The patient recalls that at the age of nine, since the injections were extremely painful, he decided that he did not want to pursue any more treatments and chose to simply live with his keloids. Over the next 5 years, his keloids continued to grow slowly, and at the age of 14, he sought care from a dermatologist who specialized in laser surgery. For the next four years, he underwent several laser treatments to both his ears.
He found laser treatments extremely painful, recalling 45-minute long sessions that, despite usage of local anesthetics, caused him tremendous pain along with a very unpleasant smell of burnt flesh that filled the treatment room. At the age of 18, he gave up on laser treatments because of the associated severe pain, yet he continued with steroid injections as his sole treatment method for another 18 months. After a short gap, he presented to that author’s practice for medical care.
Treatment
When indicated, topical cryotherapy, as previously described by the author, was applied using large cotton swabs that were dipped in liquid nitrogen and applied directly to the keloid tissue with the goal of inducing total freezing of all visible keloid tissues. Since every keloid had a unique shape and configuration, attention was given to the location, shape and size of the keloid lesions. Care was given to limit the frostbite to the keloid tissue only and to avoid freezing of normal tissue. Application of liquid nitrogen was continued until the whole keloid mass was visibly frozen. Figure 2 depicts the appearance of the frozen keloid immediately after application of cryotherapy.
Prior to the treatment, all patients were educated about the procedure and the healing process and proper aftercare of the treated keloids. They were also prescribed adequate pain medications. Treatment was repeated every 6-8 weeks until the desired results were achieved.
Outcome Measures
The primary outcome was measured by the ability of cryotherapy to induce complete or near complete resolution of the target keloid lesions. It was assumed that a significant reduction in the mass of keloid lesions would result in patients’ satisfaction – taking into consideration the pain and suffering, time to achieve the results, other inconveniences that are associated with receiving medical care, as well as associated costs. The treatment course was considered complete either when patients announced their satisfaction with the results or when there was no residual keloid left to treat.
Statistical Analysis
Due to the small sample size of this report, descriptive statistics were used. Raw data is provided in simple tables to allow better understanding of the study cohort and treatment outcomes.
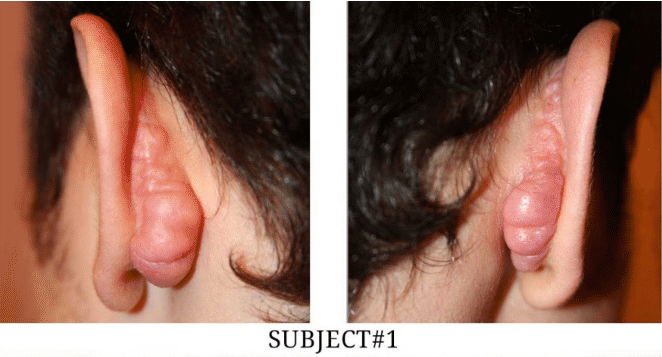

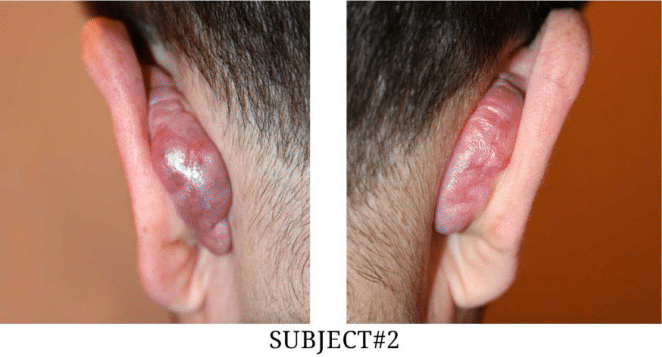

FIGURE1: Four Cases of Bilateral Post-Otoplasty Keloids.
One patient required two courses of cryotherapy to achieve desired results. Three patients received four courses of cryotherapy and were happy with their outcomes. Another patient who had very large bilateral keloids at presentation required six courses of treatment to achieve near complete remission. This particular patient presented 23 months later with minimal bilateral keloid recurrence in the upper poles of both ears. He is currently undergoing repeat cryotherapy for the recurrence. Figure 4 depicts the size and shape of this patient’s keloids at presentation, at completion of treatment, and at recurrence. Time from presentation to achievement of the results shown in Figure 4 ranged from 6-22 months. Video 1 depicts the method of applying cryotherapy to his right ear during his first visit with the author.
Another patient who had a unilateral post-otoplasty keloid required a total of 10 treatments to achieve desired results and has been in remission now for 22 months. Treatment results are summarized in Table 2.
Another interesting finding among this group of patients was that all were Asian or Caucasian. It is well known that keloid disorder is common among African Americans. This racial disparity needs to be explored and explained. However, this disparity may be due to lack of demand for otoplasty among African Americans.

DISCUSSION
Although this report is limited to treatment of only nine patients with post-otoplasty keloids, the results achieved using cryotherapy are quite encouraging. Cryotherapy is by far less invasive and less morbid than surgical intervention.
For several decades, keloids have been known to occur after otoplasty. Although there are numerous publications describing various treatment approaches to keloids, there is a paucity of literature as to proper treatment of otoplasty induced keloids. A pubmed search yields only a few publications, all of which describe surgical treatment with excision of the keloid tissue, either using flaps or excision followed by radiation therapy. Park et al. describe treating 15 cases of auricular keloids that developed subsequent to conchal cartilage grafts. In their hands, keloid removal surgery followed by application of adjuvant magnetic discs resulted in a 93.3% non-recurrence rate with minimum of 18 months of follow up.
Ethics
The underlying research project for this retrospective study was determined by the Western IRB to meet the conditions for exemption under 45 CFR 46.101(b)(4). Consent is not required for studies that are determined to be exempt under 45 CFR 46.101(b)(4)
RESULTS
Among 13 patients (22 ears with keloids), two patients (four ears) had minimal keloid formation at the site of surgery and were advised to primarily receive, or continue with, intra-lesional steroids. Eleven patients had bulky keloids and were offered cryotherapy. Nine patients consented to treatment.
Three patients are still receiving treatment and as of their last follow up visit have achieved partial reduction in the mass of their keloids. Six patients completed their course of treatment and achieved desired results. Figure 3 depicts the before and after appearance of treated keloids in seven ears.

Cryotherapy is a non-surgical method that can successfully destroy bulky keloid tissues. Cryotherapy has been utilized with great success in treatment of ear keloids. Although there are some limitations in usage of cryotherapy for treatment of keloid lesions, this method seems to not trigger the wound healing response to the extent that surgical scalpels do.
Inducing precise frostbite in the keloid tissue results in tissue necrosis that is limited to the keloid tissue alone. Upon healing, since the integrity of the underlying tissue is unaffected, all that is needed is epithelization of the surface below the necrotic tissue.


This is in total contrast to surgery that results in a deep dermal incision, repair of which will require fibroblast proliferation and collagen production to seal the sutured wound.
RECOMMENDATION
Post-otoplasty keloids are challenging complications of a cosmetic procedure that is often performed on children and young adults. Treatment of this postoperative complication poses numerous challenges, most importantly re-induction of keloid process by attempted keloid removal surgery. As the underlying pathophysiology of keloid disorder is embedded in the wound healing response, the treatment approach should preferably be non-surgical. As demonstrated here, contact cryotherapy can be used as the primary mode of treatment for all bulky post-otoplasty keloids. This treatment approach is safe, effective, and easy to apply. Adequate pain control and patient education are two important factors in assuring patient compliance and achieving satisfactory results.
Proper utilization of cryotherapy as the primary method of treatment for bulky post-otoplasty keloids has the potential of becoming a practice changing intervention. Due to the rarity of this type of keloid, the author recommends further assessment of this intervention as the primary treatment for all post-otoplasty keloids in a properly designed randomized trial.
BIBLIOGRAPHY
- Pawar S, Koch C, Murakami C. Treatment of prominent ears and otoplasty: a contemporary review. JAMA Facial Plast Surg. 2015;17:449-454.
- Calder JC, Naasan A. Morbidity of otoplasty: a review of 562 consecutive cases. Br J Plast Surg. 1994;47:170-174
- Nazarian R, Eshraghi AA. Otoplasty for the protruded ear. Semin Plast Surg. 2011 Nov; 25:288-294.
- Marneros AG, Norris JE, Olsen BR, Reichenberger E. Clinical genetics of familial keloids. Arch Dermatol. 2001 Nov;137:1429-34.
- Tirgan MH, Shutty CM, Park TH. Nine-month-old patient with bilateral earlobe keloids. Pediatrics. 2013 Jan;131:e313-317.
- Tirgan MH. Massive ear keloids: natural history, evaluation of risk factors and recommendation for preventive measures - a retrospective case series. F1000Research 2016,5:2517.
- Pérez A, Escudero F. Bilateral keloids secondary to otoplasty treated by excision and keloids flaps. An Sist Sanit Navar. 2013 Sep 6;36:333-338
- Carvalho B, Ballin A, Becker R, et al. Treatment of retroauricular keloids: revision of cases treated at the ENT service of HC/UFPR. Int Arch Otorhinolary ngol. 2012 Apr;16:195-200.
- Park TH, Park JH, Kim JK, et al. Analysis of 15 cases of auricular keloids following conchal cartilage grafts in an Asian population. Aesthetic Plast Surg. 2013 Feb;37:102-105.
- Rusciani L, Paradisi A, Alfano C, Chiummariello S, Rusciani A. Cryotherapy in the treatment of keloids. J Drugs Dermatol. 2006 Jul-Aug;5:591-595.
- Fikrle T, Pizinger K. Cryosurgery in the treatment of earlobe keloids: report of seven cases. Dermatol Surg. 2005 Dec;31:1728-31.
- Camacho-Alonso F, López-Jornet P, Bermejo-Fenoll A. Effects of scalpel (with and without tissue adhesive) and cryosurgery on wound healing in rat tongues. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2005 Sep;100:e58-63.
